
When a toothache, a knocked-out tooth, or a broken restoration happens, the minutes and hours that follow matter. Start by staying calm and collecting any fragments of tooth or restoration you can find; preserving pieces can make repair easier. Rinse the mouth gently with warm water to remove debris, and use a clean cloth or gauze to control bleeding. Avoid probing the wound with your fingers or hard instruments.
If a tooth has been dislodged but not completely knocked out, try to keep it in its socket and call for urgent care. For a completely avulsed tooth, handle it by the crown (not the root), and if possible place it back in the socket or store it in milk or saline until you can be seen. Over-the-counter pain relievers and a cold compress applied to the outside of the cheek can help control discomfort and swelling while you arrange for treatment.
Certain actions can make a situation worse, so do not place aspirin directly on an aching tooth or try to force a fractured tooth back into place. Avoid hard or chewy foods on the affected side and do not attempt complex home repairs. If there is severe bleeding, altered consciousness, or facial trauma beyond the mouth, seek emergency medical care immediately; dental teams coordinate with medical providers when injuries involve the jaw, airway, or significant facial structures.
Dental emergencies come in many forms, from sudden, sharp pain to swelling and infection. A severe toothache may signal deep decay, a cracked tooth that reaches the nerve, or an abscess — an infection around the root that can cause throbbing pain, fever, and facial swelling. Broken or fractured teeth can expose sensitive inner tissues and increase risk of infection if left untreated.
Other urgent problems include lost or dislodged crowns and fillings, which can expose the underlying tooth and create sharp edges that irritate soft tissues. Wisdom tooth flare-ups often present as localized pain, swelling, and limited mouth opening; these can escalate quickly and require prompt evaluation. Prosthetic issues such as broken dentures or loose partials also qualify as urgent when they impede chewing or cause tissue soreness.
Soft-tissue emergencies — lacerations, swelling, or infections of the gums, cheeks, tongue, or lips — deserve careful attention as well. Oral infections can be bacterial, viral, or fungal in origin and may present with redness, pustules, or persistent soreness. Early assessment helps determine whether antibiotics, local treatment, or referral to a specialist is necessary.
Recognizing the difference between minor discomfort and true urgency can guide your response: uncontrolled pain, rapidly increasing swelling, difficulty breathing or swallowing, and uncontrolled bleeding are signals to seek immediate care rather than waiting for a routine appointment.
When you arrive for emergency care, the clinical team focuses on rapid assessment and stabilization. This begins with a focused history to understand how the injury or pain began, followed by a targeted clinical exam. Vital signs and a review of any medical conditions or medications help determine the safest treatment pathway. Triage prioritizes conditions that threaten airway, bleeding control, or the viability of teeth and surrounding tissues.
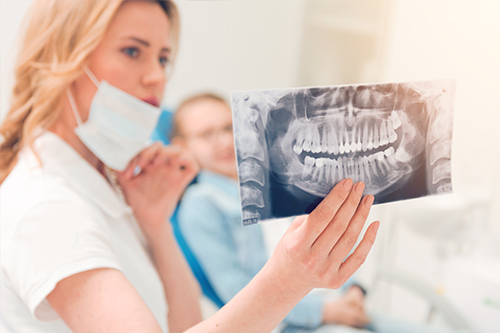
Diagnostic imaging plays a key role in emergency evaluation. We use contemporary tools such as digital radiography and cone beam computed tomography (CBCT) when indicated to visualize root anatomy, fractures, and the extent of infection. Imaging helps clinicians plan precise interventions — for example, deciding whether a tooth can be saved with root canal therapy or whether extraction is the safer option.
Stabilization focuses on reducing pain and preventing progression. That may include temporary restorations, gentle reshaping of sharp edges, suturing soft-tissue injuries, or prescribing short courses of medication when infection or severe inflammation is present. The goal during the initial visit is not always definitive reconstruction; instead, the team aims to secure comfort, manage infection risk, and outline a timely plan for definitive care.
Treatment varies with the condition and its severity. Minor fractures or lost fillings are often corrected with bonding materials or new restorations to restore form and protect the tooth. Larger structural damage may require a crown to rebuild strength and function. When the tooth’s nerve is involved, root canal therapy can eliminate infection and preserve the natural tooth; this approach is commonly recommended to avoid extraction when feasible.
In cases where a tooth cannot be saved due to extensive fracture, severe infection, or structural failure, extraction becomes necessary. Modern extraction techniques prioritize comfort and tissue preservation, and the team discusses replacement options to restore chewing ability and esthetics. Immediate repairs to dentures or temporary prosthetics can often be completed to maintain daily function while a longer-term restoration is planned.
For replacement of missing teeth, options range from conventional bridges and removable partials to dental implants. Implants are a durable solution for many patients and can reestablish a natural appearance and function, but the appropriate choice depends on clinical factors including bone availability and overall health. Care plans always consider the patient’s goals and long-term oral health.
When infection is present, targeted therapy includes drainage when required and the judicious use of antimicrobial agents in conjunction with mechanical treatment. Pain control strategies include localized anesthesia for procedures and stepwise guidance on appropriate analgesics for home use, enabling safe recovery and follow-up care.
Expect a focused, efficient appointment that addresses your immediate needs and lays out next steps. After triage and evaluation, the clinician will explain findings, proposed interventions, and any follow-up required to complete definitive care. If advanced imaging or specialist input is needed, the team will coordinate those next steps so treatment progresses without unnecessary delay.
After emergency treatment, follow-up instructions cover wound care, diet modifications, and signs that warrant an earlier return visit — increasing pain, persistent fever, or worsening swelling are important to report. Typical aftercare may include temporary dietary adjustments, oral hygiene recommendations to promote healing, and a schedule for definitive restorative visits. If medications are prescribed, follow the directions carefully and notify the office of any adverse reactions.
For those concerned about anxiety or comfort during urgent procedures, our clinicians can discuss options for local anesthesia or other measures to help you remain relaxed during care. Clear communication about expectations and recovery timelines helps patients regain comfort and function quickly and safely. At Murphy Dentistry, we aim to make emergency visits as straightforward and reassuring as possible.
In summary, dental emergencies require prompt, informed action to relieve pain, prevent infection, and preserve oral function. Quick first aid, timely professional assessment, and an appropriate treatment plan together limit complications and support the best possible outcome. Contact Murphy Dentistry for more information about emergency dental services or to arrange prompt evaluation; our team is prepared to help when urgent dental needs arise.

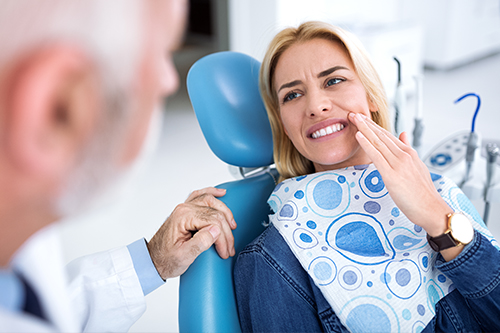
Pain is your body's way of signaling that something is not quite right and though there are many reasons for oral pain, one of the most common complaints and reasons for seeking urgent dental care is a toothache. Whether you simply need a dental filling, a crown, or require a root canal procedure to save your tooth, we'll alleviate your discomfort and restore the look and function of the involved tooth.
Dental trauma can result in a defect as minor as a small chip in tooth enamel to a more extensive and painful crack or fracture. With sufficient force, a tooth can even be displaced or completely knocked out of its socket. With prompt emergency care, many injured teeth can be restored and saved.
The last teeth in your mouth to develop, wisdom teeth often do not have enough room to fully erupt or may be positioned in the wrong direction. These issues can affect your dental health as well as overall well-being. Our office provides skilled care to address the complications caused by problematic wisdom teeth.

A broken or lost dental prosthesis or restoration can cause embarrassing gaps in your smile as well as compromise your ability to eat and speak with ease. If you've lost or broken a dental filling, denture, crown, or other dental appliance, you can rely on our office to perform a prompt repair or provide a durable and cosmetically pleasing replacement as quickly as possible.
At the office of Murphy Dentistry, emergency appointments are always available. Of course, in addition to providing top treatment for dental emergencies, we also welcome patients searching for high quality and affordable care. We offer a complete range of the latest and best cosmetic and dental services for every member of your family.
If you are suffering from a toothache or have sustained a dental injury, it is important to visit the dentist as soon as possible before more serious complications arise. Whether your dental emergency is painful, if it affects the appearance of your smile, or if you suspect that an infection is present, our office will make every effort to see you as promptly as possible for care.
At the office of Murphy Dentistry, we treat your dental emergency as our top priority. Our caring team will respond to your emergency call right away, making sure you get the gentle, state-of-the-art care you need without delay.
As your trusted emergency dentist in Loxley, we provide the highest quality of care to mitigate the stress, anxiety, and discomfort of dental problems. Our dedicated team will help you start feeling better as soon as we receive your emergency call.
At the office of Murphy Dentistry, we provide skilled and experienced care to effectively resolve a broad range of dental emergencies, restoring a patient's oral health while protecting their overall wellbeing.
However, even so, specific dental emergencies pose significant threats to one's health. These situations require immediate, emergency room care. Serious and potentially life-threatening dental emergencies include significant oral and facial trauma such as jaw fractures, deep wounds or lacerations to the face and mouth, an abscess or infection that causes widespread facial or submandibular swelling, or affects breathing and swallowing.
At the office of Murphy Dentistry, we provide prompt, skilled, and experienced care to address dental emergencies. We understand that finances are always a concern and do our best to provide options in care that are both affordable and respect your budget.
Once we've had the opportunity to examine your smile, we can give you a clear picture of any existing dental issues, along with a quote for what the cost of treatment will be. The cost of care all depends upon the extent and complexity of issues affecting the health or appearance of your smile and the types of procedures that are required.
To help alleviate any additional stress or delay, you can count on our staff to work with you to optimize coverage for your dental care and to minimize your out-of-pocket expenses. For patients without insurance, we strive to make things easier as well! We invite you to visit our financial information page or speak to an expert in our business office.
Dental emergencies are often painful and debilitating experiences. For this reason it's important to have an emergency dentist in Loxley, who welcomes patients with urgent dental needs while providing the prompt care required to restore oral health.
Here are just some of the reasons why so many patients choose our office for emergency dental care and to meet their family's dental needs:
We're dedicated to helping patients enjoy good oral health and beautiful smiles. We look forward to helping you keep your smile in tip-top condition. You can rest assured that our highly skilled office team will provide you the highest quality of state-of-the-art dental care and have you smiling again in no time!
To make an appointment or for more information on our office and the many state-of-the-art services we provide, give us a call today.

Taking the next step toward your ideal smile is simple. Whether you're ready to schedule your appointment or simply have questions about our services or treatment options, our friendly staff is here to help.